Rural Hospital Funding Cuts: Montana Faces Healthcare Crisis
Federal funding changes threaten rural hospitals in Montana, potentially leading to service cuts and healthcare access issues. Explore the implications for patients and the future of rural healthcare.
Montana Rural Hospitals Face Potential Service Cuts Due to Federal Funding Changes
Rural hospitals across Montana are facing a challenging situation. Changes in federal funding models could lead to significant service cuts, jeopardizing access to crucial healthcare for residents in these underserved communities. This is especially concerning for small facilities like Big Sandy Medical Center, where resources are already stretched thin.
The Situation at Big Sandy Medical Center
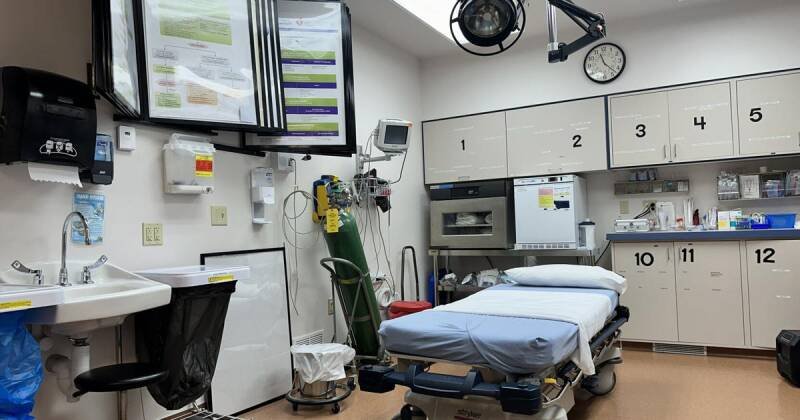
Big Sandy Medical Center, a 25-bed rural hospital, vividly illustrates the challenges. Its emergency department, a single room separated by a curtain, highlights the need for facility updates. Former CEO Ron Wiens has emphasized the critical need to modernize the infrastructure.
The potential funding cuts could severely impact the hospital's ability to provide essential services, including emergency care, routine checkups, and specialized treatments. This could force residents to travel long distances for medical care, adding to their burden and potentially delaying crucial interventions.
Why This News Matters
This news is significant for several reasons:
- Impact on Patient Access: Reduced funding directly translates to reduced services. This could mean longer wait times, fewer available specialists, and even closure of essential departments like the emergency room.
- Economic Consequences: Rural hospitals are often major employers in their communities. Cuts could lead to job losses, further straining the local economy.
- Health Disparities: Rural residents already face significant health disparities compared to their urban counterparts. Funding cuts will exacerbate these disparities, making it even harder for them to access quality care.
Our Analysis
In our opinion, the current funding model inadequately addresses the unique challenges faced by rural hospitals. These facilities often operate on tight margins and serve a dispersed population, making it difficult to generate sufficient revenue. The reliance on Medicare and Medicaid reimbursements, coupled with rising operational costs, creates a perfect storm. Changes to federal policy need to acknowledge that one-size-fits-all funding solutions rarely work.
The emphasis seems to have shifted towards efficiency and value-based care, which, while important, may not be achievable for rural hospitals operating with limited resources. We believe that a more nuanced approach is needed, one that considers the specific needs and circumstances of rural communities.
The Role of Federal Funding
Federal funding plays a vital role in supporting rural hospitals. Medicare and Medicaid reimbursements are crucial sources of revenue, and any changes to these programs can have a ripple effect. These policy changes often stem from an effort to reduce healthcare costs. This highlights the ongoing tension between controlling spending and ensuring equitable access to healthcare for all Americans.
Future Outlook
The future of rural healthcare in Montana hinges on several factors, including:
- Federal Policy Decisions: Congress and federal agencies will play a key role in shaping the future of rural healthcare funding. Advocacy and lobbying efforts by rural hospital associations will be crucial.
- State Government Support: State governments can provide supplemental funding and implement policies to support rural hospitals. This could include tax incentives, grants, and other forms of financial assistance.
- Community Involvement: Strong community support is essential for the survival of rural hospitals. Local residents can advocate for their hospitals, volunteer their time, and donate to support their operations.
Potential Solutions
This could impact healthcare innovation and alternative delivery models like telehealth. Telehealth can extend access to specialists and reduce the need for travel. But it requires significant investment in infrastructure and training, and reimbursements for telehealth services are not always adequate.
In conclusion, the potential funding cuts facing rural hospitals in Montana represent a serious threat to healthcare access. Addressing this challenge will require a multi-faceted approach involving federal, state, and local stakeholders. Failure to do so will only widen health disparities and jeopardize the well-being of rural communities.