Rural Hospital Funding Cuts Loom: Impact on Emergency Care and Future Outlook
Federal funding changes threaten rural hospitals like Big Sandy Medical Center. Understand the potential impact on emergency services, healthcare access, and the future of rural healthcare.
Rural Hospital Funding Cuts Loom: Impact on Emergency Care and Future Outlook
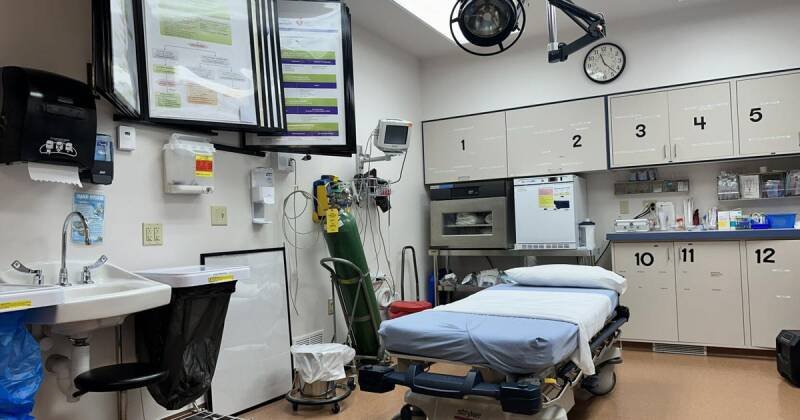
Big Sandy Medical Center, a vital healthcare hub in rural Montana, exemplifies the challenges facing critical access hospitals across the nation. Its emergency department, a single room with limited resources, highlights the need for updates and investment. However, potential changes in federal rural health funding could force service cuts, jeopardizing access to crucial medical care for rural communities.
The Situation at Big Sandy Medical Center
Big Sandy Medical Center, like many rural hospitals, operates on thin margins. They rely heavily on federal funding programs designed to support healthcare access in underserved areas. This funding helps them maintain essential services, including the emergency department and other crucial medical departments.
Former CEO Ron Wiens emphasized the facility's critical role in the community, highlighting the need for upgrades and the potential ramifications of funding reductions. The hospital serves as a lifeline for residents, providing everything from emergency care to basic check-ups.
Why This News Matters
The potential loss of federal funding for rural hospitals isn't just a financial issue; it's a matter of life and death for those living in rural areas. These hospitals are often the only source of medical care for miles, providing essential services that larger, urban hospitals simply can't offer. Cuts could lead to:
- Reduced access to emergency care, potentially increasing mortality rates.
- Loss of vital services like obstetrics, leaving pregnant women with limited options.
- Increased travel times for medical care, creating additional burdens for patients.
- Closure of hospitals, further isolating rural communities.
Our Analysis
The crux of the issue lies in the complexities of Medicare reimbursement and the way rural hospitals are designated and funded. Changes in how Medicare classifies and pays these facilities could have a devastating impact on their financial stability. In our opinion, policymakers need to carefully consider the unintended consequences of these changes and prioritize the needs of rural communities.
These rural hospitals, often designated as "Critical Access Hospitals" (CAHs), receive enhanced reimbursement rates to compensate for their smaller size and lower patient volume. However, some argue that these enhanced payments are unsustainable. The debate centers on finding a balance between fiscal responsibility and ensuring equitable access to healthcare, regardless of location.
The Impact on Communities
Beyond healthcare, rural hospitals are often significant employers in their communities. Reductions in services or hospital closures can lead to job losses, further straining local economies and contributing to a decline in population. This creates a vicious cycle, where dwindling resources lead to reduced services, further driving away residents and businesses.
Future Outlook
The future of rural healthcare hinges on the decisions made by federal and state policymakers. Several potential solutions could help mitigate the negative impacts of funding cuts:
- Telemedicine Expansion: Leveraging technology to provide remote consultations and monitoring.
- Increased Collaboration: Forming partnerships between rural and urban hospitals to share resources and expertise.
- Targeted Funding: Developing funding models that specifically address the unique challenges faced by rural hospitals.
- Community Involvement: Engaging local residents in the planning and decision-making processes related to healthcare.
This could impact a whole spectrum of rural life. In our opinion, a collaborative approach is necessary to secure the future of rural healthcare. Without it, communities like Big Sandy face a bleak prospect, struggling to provide even the most basic medical services to their residents.
The situation requires immediate attention and a commitment to finding sustainable solutions that prioritize the health and well-being of rural Americans.